The Use of a Mesenchymal Stem Cell Living Skin Substitute in Conjunction with Topical Wound Oxygen for an lschemic Post Operative Transmetatarsal Amputation
Francis Derk, DPM, CDR USN STVHCS: Chief Podiatry Services UTHSC: Assistant Clinical Professor
A 66 yr/o Male with a hx of severe PVD, CVA, CHF, Hep C, s/p BKA, End Stage Renal Dx, and DM Underwent a TMA of the
Left foot secondary to Osteomyelitis and infection. Immediately post operatively, the wound became escharotic and dehisced. The patient was then placed on Topical Wound Oxygen Therapy (TW02) for wound staging and wound bed preparation.
The patient underwent a Vascular Bypass Graft 5 months prior to the TMA procedure. Pre and Post NIVs were N/C. The patient was not a candidate for further vascular surgery and presented with a natural hx of limb loss on the contralateral side prior secondary to PVD and infection.
ABls: Left Not compressible (N/C) TBls: (TMA)
S/P: SFA-PTA Bypass Non palpable pulses Dopplers: non audible Waveforms: flat line
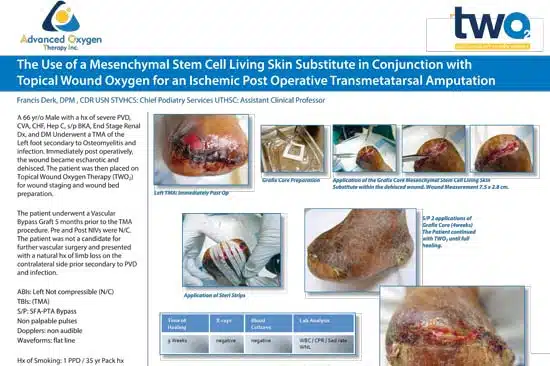
Left TMA: Immediately Post Op
Grafix Core Preparation Application of the Grafix Core Mesenchymal Stem Cell Living Skin
Substitute within the dehisced wound. Wound Measurement 7.5 x 2.8 cm.
Hx of Smoking: 1 PPD / 35 yr Pack hx
A 47 yr/o Female with a hx of severe DM, Retinopathy, and Neuropathy presented to the Emergency Department with a severe eft foot infection. The patient presented very confused and had not seen a provider in over a year. She stated the ulcer started as a ister on the bottom of her foot and was receiving care by her immediate family.
A multidisci inary team approach was attained and cllaboration was estaished with Medicine, Vascu ar Surgery, and nfectious Disease. The patient had pa pable pulses (2/4) and were audible upon bedside testing. The patient presented with a 560g ucose ev a ong with normocytic anemia with an H/H of 7.9/25.3. Two units of packed RBCs were given during surgery and 2 more units were given at post op day 1. The patient had a spike in her WBC at post op day 1 which was attributed to the transfusion.
A negative pressure device was used for 3 days and then discontinued due to pain and discomfort. Topica Wound 01 therapy was initiated fowing surgery bid for 90 mins.
The patient was discharged on post op day 6 and was aced on po Augmentin 500/125 mgs bid for 14 days. Wound dressings consisted of ight wet to dry packing changed bid in conjunction with TWO1 therapy bid/90 mins. The patient was aced in a removable posteriors int for 3 weeks and then transitioned to a CAM boot unti hea ed. Once healed, the patient was aced into a custom molded shoe with tier.
Conclusion: This is a very complicated case of a Diabetic Foot infection that responded favorably to a multidisciplinary approach and Topical Wound 02 Therapy. The TWO2 was very effective not only from a wound healing perspective, but also in providing the patient with comfort, direct involvement with her wound care, and ease of use at home.